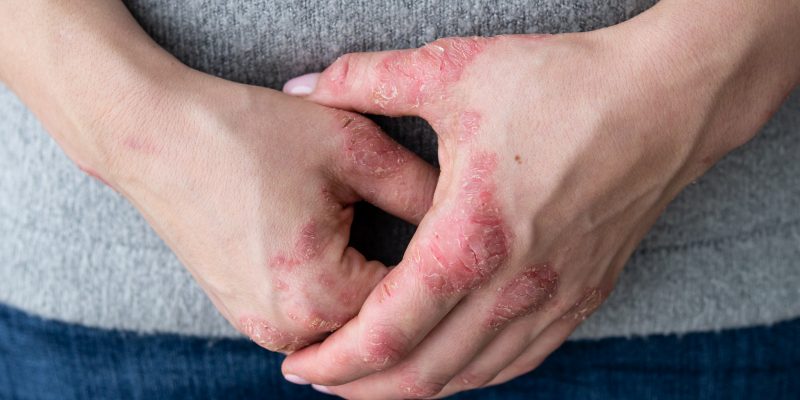
Psoriatic arthritis (PSA) is a chronic autoimmune disorder. That is a condition in which the body’s immune system attacks healthy cells. As a result, this leads to joint damage and most often a skin condition called psoriasis. While not all people develop PSA after being diagnosed with psoriasis, it is common. ¹
In the spine, its called spondylitis and causes stiffness in the back, neck, and hips. Additionally, it causes tender spots where tendons and ligaments join onto bones called enthesitis. The most common areas for enthesitis are in the back of the heel, the sole of the foot, and around the elbows. Enthesitis is one of the characteristic features of psoriatic arthritis. ²
Symptoms
The primary symptoms of psoriatic arthritis are stiffness, tenderness, swelling, and pain in the joints. In particular, the fingers, toes, feet, and lower back are affected. Since it is closely related to psoriasis, typically red sink patches called psoriasis develop first. In more severe cases, skin lesions may appear. PSA is a disease that tends to flare and subside, so symptoms may not always be present.

Causes
PSA is believed to be caused by an overactive or abnormal immune system. As a result, the body attacks healthy cells and tissues. Additionally, and in the case of psoriasis (PSO), the body’s response causes the overproduction of skin cells.
Furthermore, some research indicates that environment plays a factor in the activation of PSA. This includes other infections, such as strep throat.
Treatment
PSA treatment is typically handled by a Rheumatologist or general practitioner. Since many patients have psoriasis also, it’s not uncommon for a dermatologist to first recognize and refer patients who develop this form of arthritis.
There is no cure for PSA, so treatments are for the symptoms only.
One option is biologic medications. These tend to be more selective in blocking the inflammation of PSA. Treatment may also be with anti-inflammatory drugs, disease-modifying antirheumatic drugs (DMARDs), immunosuppressants, or steroids. ³
References
1. https://www.mayoclinic.org/diseases-conditions/psoriatic-arthritis/symptoms-causes/syc-20354076
2. https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Psoriatic-Arthritis
3. https://www.webmd.com/arthritis/psoriatic-arthritis/psoriatic-arthritis-the-basics#1